Researchers investigate a new way to detect small airway damage in COPD
Author

Dr. Dragos M Vasilescu, PhD Research Associate, Dept of Pathology & Laboratory, UBC; Centre for Heart Lung Innovation at Providence Health Care (St. Paul’s Hospital)
Chronic obstructive pulmonary disease (COPD) affects over 2 million Canadians and is the major cause of hospital admissions of adult males and increasingly females over 40 years of age in Canada.
More than 50 years ago, Canadians working at McGill University in Montreal were the first to show that the major site of airflow obstruction in COPD is located in the small airways in the lung. Last year, researchers at the Centre for Heart Lung Innovation (HLI), located at St Paul’s Hospital, have shown using the latest imaging technologies with unprecedented resolution that the small airways deep within the lungs are destroyed before any clinical symptoms or abnormalities can be observed (Lancet Respiratory Medicine).
We know now that once airways are damaged, it is generally irreversible and will continue to progress, even for those who quit tobacco products. Unfortunately, today’s available treatments for COPD are mostly directed at relieving symptoms by dilating constricted airways or treating inflammation, but nothing is designed to reverse the disease responsible for the airway obstructions. Therefore, early detection of airway abnormalities would be key for any successful treatment.
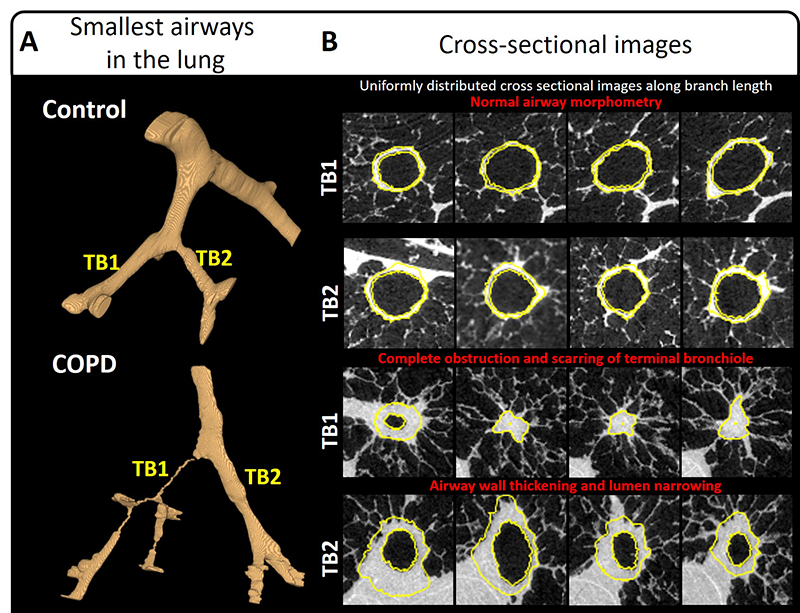
For his work, Dr. Vasilescu used a micro CT scanner located at the HLI and software that he and his colleagues have developed to image and measure the disease present in the smallest airways in the lung. This new study has been published in the American Journal of Respiratory and Critical Care Medicine.
It is the hope of the whole group that this novel technique provides a way to accurately identify patients who are most likely to progress to symptomatic lung disease before they can be diagnosed with traditional methods such as pulmonary function tests, ensuring earlier and more effective treatment for the patients. This study could revolutionize how new therapies for COPD and potentially other lung diseases are developed.

