Within ten days of China releasing the SARS-CoV-2 genome, the BCCDC PHL created a nucleic acid test and began to offer testing. It then shared the test protocols, reagents, and provided guidance to other front-line laboratories in BC and Canada.
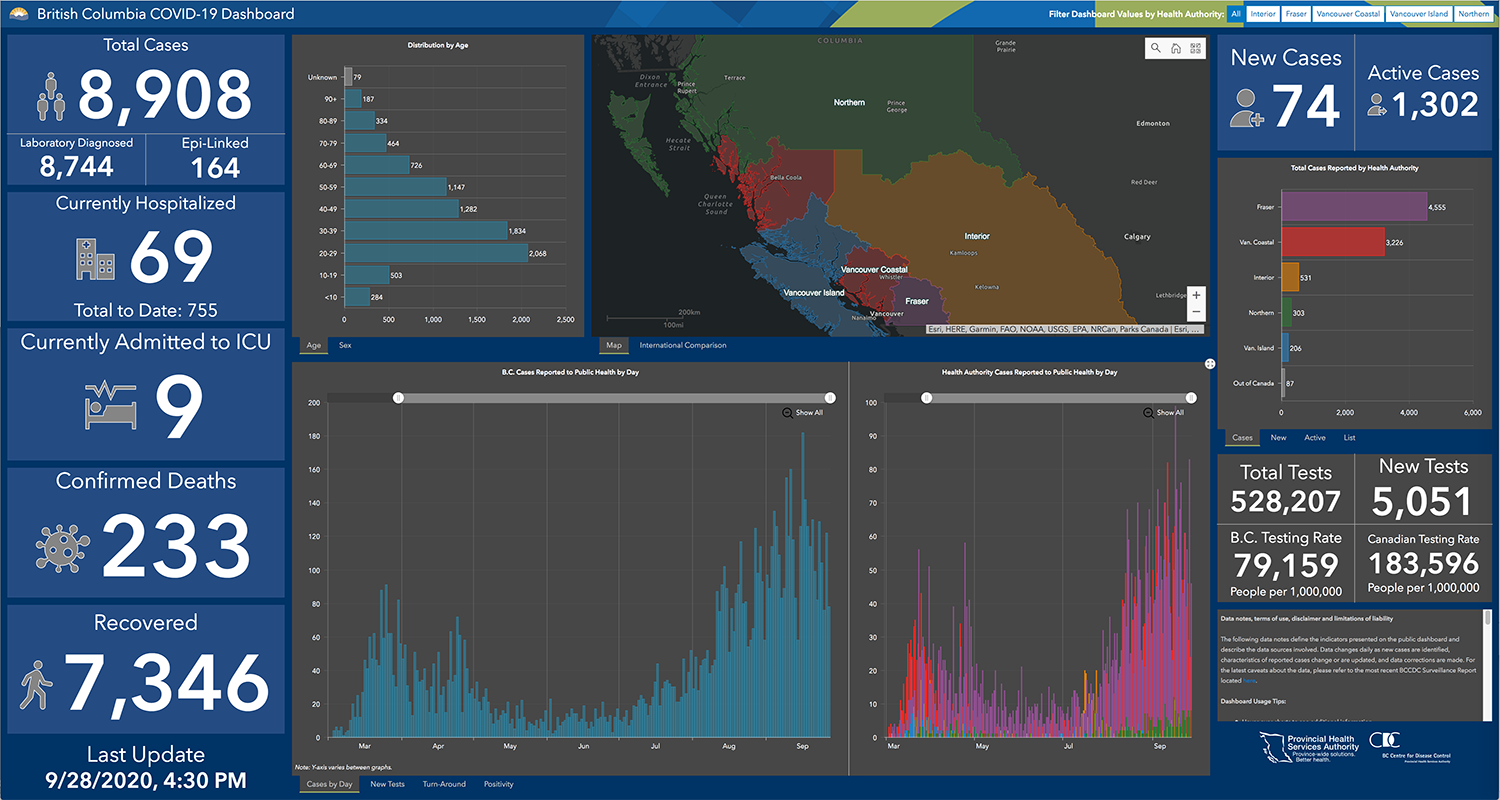
Since January, B.C. laboratories have conducted more than 506,000 tests.
Two days after Dr. Bonnie Henry, the Provincial Health Officer for British Columbia, arrived at the BCCDC to inform the media of the province’s first confirmed case, Genome BC provided research funding to start sequencing SARS-CoV-2 from patient samples. This allowed us to determine if new cases were part of a known outbreak or the strain was derived from a newly imported case. It also helped monitor COVID-19 cases connected to a Vancouver dental conference and highlighted the potential impact of mass gatherings in spreading the virus.
To date, members of the Department of Pathology and UBC who work at the BCCDC have been successful in leading numerous research projects such as creating step-by-step self-collection kits for remote tree planters, evaluating COVID-19 serology, working on integrating provincial test result data in real-time–an unparalleled amount of work.
These successes have come from decades of experience and teamwork dealing with numerous novel pathogens and previous epidemics, including: SARS, MERS, West Nile virus, Ebola, H1N1, Hepatitis C, HIV, Syphilis, Zika, as well as seasonal influenza, food, and waterborne outbreaks. For example, the foundational work for integrating the provincial COVID-19 negative and positive test results in real time came from repurposing our PLOVER database which had been developed to integrate data on carbapenemase producing organisms (CPOs) and enteric pathogens. Solid science is always built on the shoulders of others and a solid pandemic response depends on teamwork across medical, clinical, scientific, and operational domains.
Diseases do not respect jurisdictional boundaries and COVID-19’s rapid worldwide spread is a reminder of that. Yet British Columbia and much of Canada have mounted a robust COVID-19 response. This has only been possible through stakeholders working together to support each other and share expertise. The BCCDC Public Health Laboratory has strived to be a model of collaborative working in its response to this pathogen of public health importance. Testing for COVID-19 is a prime example of that. Rather than trying to centralize testing at one site after developing the SARS-CoV-2 real-time PCR assay, the BCCDC PHL rolled out the protocol to other hospital testing sites throughout the province and beyond, as well as sharing it with the private sector, to maximise capacity.
After that, we worked with our St Paul’s and Children and Women Hospital laboratory colleagues to evaluate all the SARS CoV-2 chemiluminescence antibody testing products. Colleagues from both Surrey Memorial Hospital and Vancouver General Hospital offered samples. This rapid collaboration placed BC in the national lead, but we then shared these results with our national partners. Recently, the Federal Immunity Task Force published a SARS CoV-2 national serology guidance document with participants from the Canadian Public Health Laboratory Network, Canadian Association of Microbiology and Infectious Diseases, Association of Medical Microbiology and Immunology; Canadian Association of Clinical Chemists (https://www.cmaj.ca/content/cmaj/192/34/E973.full.pdf).
In addition, the BCCDC PHL has played a key role in policy development. This includes several BC policy documents such as serology guidance documents, FAQ, SARS-CoV-2 testing, collaborating with PICNet on protocols and documents, as well as leading development of COVID-19 associated IPAC guidelines and policies.
Beyond traditional service, the BCCDC PHL is also evaluating more innovative approaches for COVID-19 serology testing, such as the use of Dried Blood Spots to test for SARS Cov-2 serology in hard to reach and incarcerated population, with provincial and national partners. In collaboration with Dr. David Goldfarb at BC Children’s and Women’s hospital, Dr. Hoang has validated and is currently implementing saline gargle in BC as a swab-independent collection method for COVID-19. This not only holds the promise of making COVID-19 sampling much easier for the patient (compared to a nasopharyngeal swab) but mitigates the challenge of global supply of nasopharyngeal swabs for testing.
While COVID-19 affects us all, it has also brought the medical and scientific community closer together in British Columbia. COVID-19 is a shared threat that unites our efforts to protect our community. For it is only by working together will we be able to tackle COVID-19 and pandemics to come.